Why Your Hip Only Hurts When You Run (And What Actually Fixes It)
Your hip feels completely fine - until you run.
Walking? No problem. Strength training? Fine. The second you start logging miles, that deep ache on the outside of your hip shows up like clockwork.
If that's your pattern, I want to answer the question you're probably already asking yourself:
Is this just aging? Am I finally falling apart?
No. And here's what's actually going on.
The Real Anatomy Behind This Pain
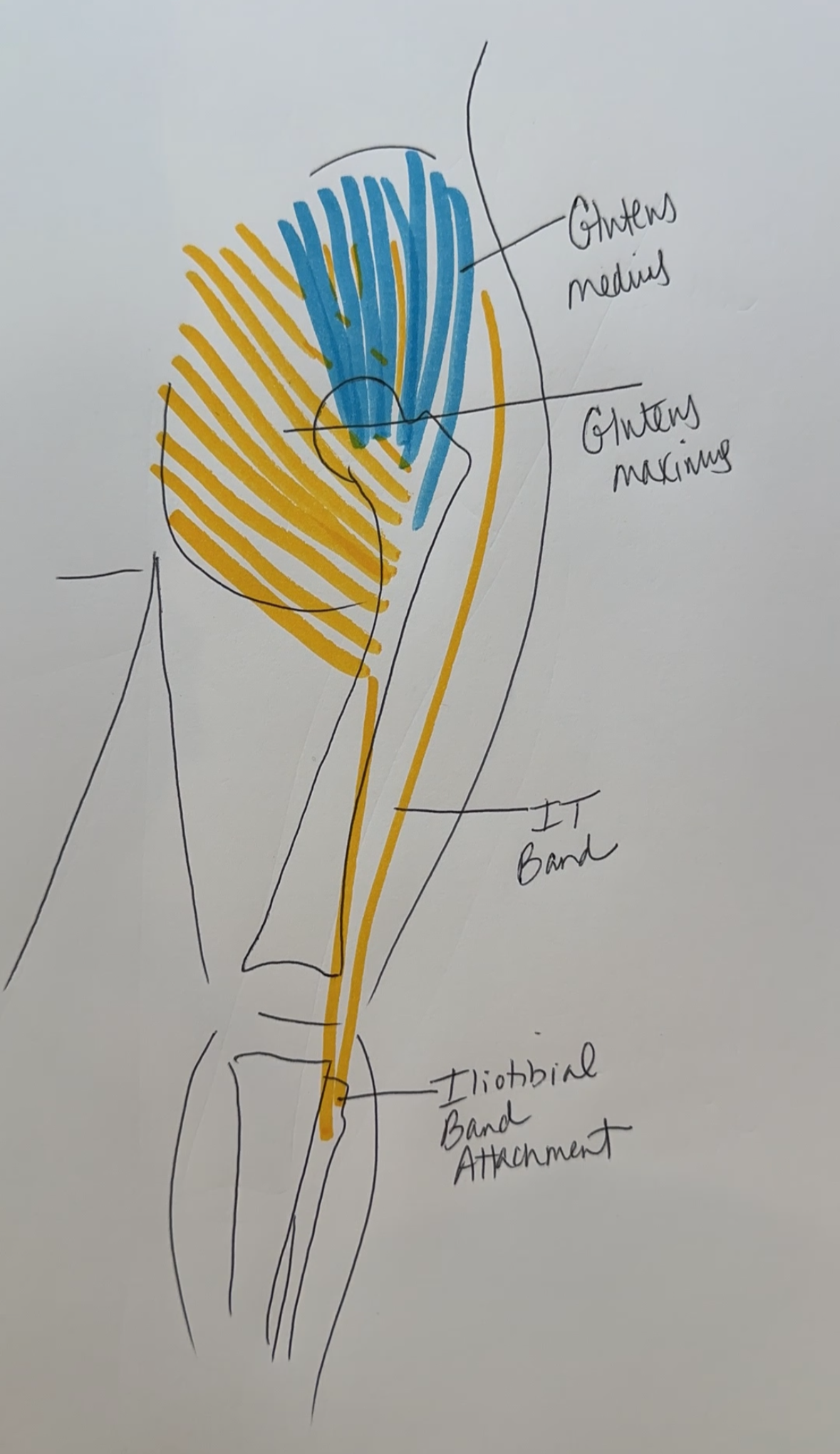
Your hip has two powerhouse muscles that matter most for running: your gluteus medius and your gluteus maximus. These aren't just any muscles - they're the primary load-bearers every time your foot hits the ground.
The gluteus medius is the one we're focused on here. It runs along the outside of your hip and narrows into a tendon that attaches to the bony point on the outside of your hip - that spot where you feel the pain.
If you're also waking up at night with a deep ache when you lie on your side, that's the same structure. The pressure of the mattress against that bony point irritates the tendon. Same problem, different position.
This condition is called greater trochanteric pain syndrome (GTPS) or “Runner’s Hip”, and it's one of the most commonly mismanaged running injuries I see in my practice.
What This Is NOT
Before we talk about what fixes it, let's clear out the noise.
It's likely not aging. Hip pain that's truly from the hip bone itself tends to show up in the groin — not the outside. If your pain is specifically on the lateral hip and only spikes with running, aging rarely explains the pain.
It's definitely not a flexibility problem. I know, everyone says to stretch. And if you've been grinding out figure-4 stretches or pigeon pose trying to get relief - you need to know that these stretches place direct compressive load on the exact tendon that's already irritated. They don't decompress it. They can make it worse.
This pain is not telling you that you need more mobility. It's telling you something else entirely.
What's Actually Happening: The Load Problem
Here's the concept that changes everything for most of my clients:
This tendon is sensitive to load - meaning the total cumulative work placed on it over time. That includes your weekly mileage, your training intensity, your daily walking, your stress levels, your sleep. All of it goes into one bucket.
Pain shows up when the load in that bucket exceeds what the tendon can recover from.
That's it. That's the core mechanism.
It's not weakness. It's not age. It's not tightness. It's a load management problem.
This is also why the pain spikes specifically when you run: the impact forces through this tendon during running are significantly higher than walking, lifting, or cycling. Your tendon is fine until it hits that threshold and running pushes it over.
Rest doesn't fix a load problem. It just temporarily removes the trigger.
When you take six weeks off and come back, the tendon hasn't gotten stronger. It's just been unloaded. The second you ramp mileage back up, the pain returns — and now you've also lost fitness. This is the cycle I see constantly.
What you need instead is relative rest paired with a deliberate plan to build the tendon's capacity.
The Two-Bucket Approach
Here's how I think about rehab for this type of pain. We work on two things simultaneously:
Bucket 1: Strength
Research is clear on this: progressive strengthening outperforms every other treatment for gluteal tendinopathy. Better than rest, better than injections, better than stretching. It's not even close.
But here's where most people go wrong — they start at the wrong place on the ladder.
Think of your strength progression like rungs on a ladder. At the bottom: a banded clamshell. A few rungs up: a glute bridge. Higher: a lunge, then a deadlift, then a heavy loaded deadlift. Each rung asks more of the tendon than the last.
If you jump straight to heavy deadlifts when your tendon is already irritated and overloaded, you're going to flare. Then you'll think strengthening doesn't work — when actually the approach just wasn't calibrated to where you are right now.
The right starting point isn't something you guess. It's something you test. Strength assessment tells you exactly where to begin so you're building capacity without spiking pain.
Bucket 2: Running Load Management
The second bucket is how you're structuring your running — what days, what distances, what intensity, and how you're introducing changes over time.
This is its own conversation, and I'm covering it in full in a follow-up video next week. Drop your questions below if there's something specific you want me to address.
The Bottom Line
If your hip only hurts when you run:
It is not a flexibility deficit
Stretching into it can make it worse
Complete rest won't solve it
Progressive strength training, started at the right level, is the most effective treatment available
This is a solvable problem. It just requires the right framework — not more guessing.
Dr. Chelsea Matthews is a Doctor of Physical Therapy with 10 years of clinical experience specializing in running injuries. She works with active adults looking for running guidance that is evidence-informed, sport-specific, and actually built around their goals.
Chelsea Matthews - Doctor of Physical Therapy, Running Specialist and Coach